Akathisia Symptom Checker
Is it akathisia or something else?
This tool helps you determine if your symptoms match akathisia, a dangerous medication side effect often mistaken for anxiety. Answer the questions honestly to get results.
When you start a new medication-especially an antipsychotic-you expect it to help your mood, thoughts, or behavior. You don’t expect to feel like you’re being pulled apart from the inside. That’s what many people describe when they develop akathisia: a crushing, unbearable urge to move, often in the legs, that doesn’t go away no matter how much they shift, pace, or stretch. It’s not just restlessness. It’s agony. And it’s frequently mistaken for anxiety, agitation, or worsening mental illness.
At the same time, another condition called restless legs syndrome (RLS) can mimic akathisia. Both make your legs feel wired, twitchy, or aching. But they’re not the same. And confusing them can lead to dangerous mistakes-like doubling your dose of an antipsychotic when you should be stopping it. This isn’t rare. Studies show up to half of people with medication-induced akathisia are misdiagnosed. The result? Increased risk of suicide, violence, or complete treatment failure.
What Is Akathisia, Really?
Akathisia isn’t just "feeling jittery." It’s a specific movement disorder caused by drugs that block dopamine in the brain. First identified in the 1950s, it’s now one of the most common side effects of antipsychotics. People on haloperidol, risperidone, or even metoclopramide (a stomach drug) are at risk. The key trigger? Starting, increasing, or suddenly stopping these medications.
It shows up fast-usually within days or weeks. You feel an inner tension, like your nerves are buzzing under your skin. You can’t sit still. You cross and uncross your legs. You rock. You shift your weight. You pace. It’s not voluntary. It’s not boredom. It’s a desperate, physical need to move. One patient described it as, "You ache with restlessness, so you feel you have to walk. And then as soon as you start pacing, the opposite occurs to you; you must sit and rest. Back and forth, up and down you go… you cannot get relief."
What makes akathisia dangerous is how often it’s misread. Doctors see someone fidgeting, pacing, or seeming "anxious" and assume their psychosis is getting worse. So they increase the antipsychotic dose. That makes akathisia worse. And worse. And worse. In one documented case, a patient on haloperidol developed acute suicidal thoughts-directly tied to akathisia. The doctor doubled the dose. The patient’s distress spiked. Only after the family insisted on a second opinion did the real cause emerge.
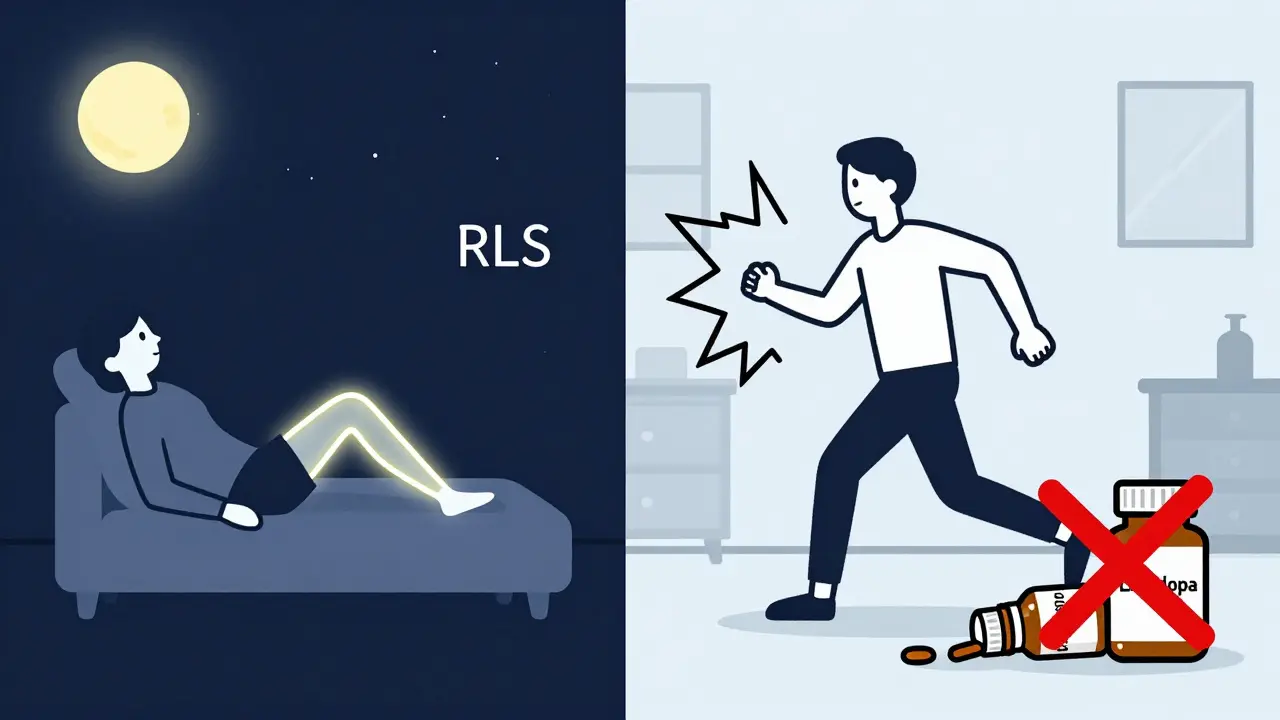
Restless Legs Syndrome: The Look-Alike
Restless legs syndrome feels similar: tingling, crawling, aching in the legs. But here’s the difference:
- RLS happens mostly at night or during rest. Akathisia hits anytime-especially while sitting.
- RLS improves with movement. Akathisia gets worse with movement, but you can’t stop moving because the discomfort is unbearable.
- RLS often runs in families or links to low iron. Akathisia links directly to medication timing.
- RLS responds to dopamine-boosting drugs like levodopa. Akathisia gets worse with them.
One person told me: "I thought I had RLS because my legs felt awful at night. But when I started risperidone, it got ten times worse during the day. That’s when I looked it up."
That’s the pattern. If your restlessness started or worsened after beginning a new medication, especially an antipsychotic, akathisia is far more likely than RLS. And if your doctor says, "It’s just anxiety," ask: "Could this be akathisia?"
How to Spot It-Before It’s Too Late
Clinicians use the Barnes Akathisia Rating Scale (BARS) to measure it. But you don’t need a scale to start asking questions. Here’s what to look for:
- Did symptoms start within 4 weeks of starting or increasing a medication?
- Do you feel an inner, unbearable urge to move-even if you’re not physically restless?
- Do you pace, rock, shift weight, or constantly adjust your legs while sitting?
- Does the feeling get worse when you try to sit still?
- Did your doctor increase your antipsychotic dose because you seemed "more agitated"?
If you answered yes to most of these, you’re likely dealing with akathisia. And if you’re on a first-generation antipsychotic like haloperidol, your risk is even higher. Second-generation drugs like quetiapine or olanzapine carry lower-but still real-risk.
What Happens If You Ignore It?
Ignoring akathisia isn’t just uncomfortable-it’s life-threatening.
- It’s linked to suicidal thoughts in 15-20% of cases.
- It can trigger aggression, outbursts, or self-harm.
- It causes 15% of people to stop their antipsychotic entirely, often without medical support.
- Some patients say the distress of akathisia is worse than their original psychosis.
A 2022 survey of 1,247 antipsychotic users found 68% were initially told their restlessness was "anxiety." Of those, 42% had their medication dose increased-making things far worse. One woman said, "They kept telling me I was paranoid. I wasn’t. I was in agony."
The longer it goes untreated, the harder it is to reverse. Chronic akathisia can last months or years. Tardive akathisia may appear even after stopping the drug. That’s why early recognition saves lives.
How to Treat It
The first rule: Don’t add more medication to fix it. That’s the trap.
Here’s what actually works:
- Reduce or stop the drug. If possible, taper the antipsychotic slowly. Haloperidol, for example, should be reduced over 3 days. This resolved symptoms in 80% of cases in clinical reports.
- Add propranolol. A beta-blocker like propranolol (10-60 mg daily) is the most studied treatment. It reduces inner restlessness and physical agitation.
- Try clonazepam. A low dose (0.5-2 mg nightly) can help, especially for sleep disruption.
- Use cyproheptadine. An antihistamine that blocks serotonin, sometimes used off-label with success.
Important: Avoid dopamine agonists like levodopa. They help RLS but make akathisia worse. Don’t treat akathisia like RLS.
For people who can’t stop their antipsychotic-say, because they have severe schizophrenia-doctors may add propranolol or clonazepam while keeping the antipsychotic. It’s not ideal, but it’s better than worsening the condition.
What’s New in Treatment?
Research is moving fast. In 2023, a new drug called pimavanserin (Nuplazid), originally for hallucinations in Parkinson’s, showed a 62% reduction in akathisia symptoms in a clinical trial. It’s not FDA-approved for this yet, but it’s being studied.
Non-drug approaches are also emerging. A 2024 pilot study at Harvard tested transcranial magnetic stimulation (TMS) on akathisia patients. Early results showed reduced restlessness after just five sessions.
And technology is helping. The Akathisia Recognition and Management App, launched in 2023 by the Movement Disorder Society, gives clinicians a quick checklist and treatment guide right on their phone. Stanford’s AI tool can now detect akathisia from video calls with 89% accuracy-meaning telehealth patients won’t be missed.
What to Do If You Suspect It
If you’re on an antipsychotic and feel this kind of inner torment:
- Write down exactly when the symptoms started-date and time.
- Track what makes it better or worse. Does sitting make it worse? Does walking help temporarily?
- Print out the Barnes Akathisia Rating Scale (available online) and bring it to your doctor.
- Ask: "Could this be akathisia? I’ve read it’s common with antipsychotics."
- If your doctor dismisses you, ask for a referral to a movement disorder specialist or psychiatrist with experience in side effects.
Don’t wait. Don’t assume it’s "just anxiety." This is a medical emergency disguised as a mood issue.
Why This Matters Beyond the Individual
Only 37% of U.S. psychiatric clinics routinely screen for akathisia. Most EHR systems don’t even have a checkbox for it. That’s not negligence-it’s ignorance. And it’s costing lives.
Pharmaceutical companies are starting to respond. New drugs like lumateperone (Caplyta) have akathisia rates under 4%, compared to 14% for older drugs. That’s progress. But until every prescriber learns to recognize this, patients will keep suffering.
Education is the missing link. Medical schools barely teach akathisia. Primary care doctors don’t know it exists. Patients are left to Google it themselves-like the Reddit user who found the answer on Wikipedia after being told it was "just anxiety."
It doesn’t have to be this way. Akathisia is recognizable. It’s treatable. And when caught early, it can vanish in days.
Can akathisia happen with antidepressants?
Yes. While most common with antipsychotics, akathisia can also occur with SSRIs like fluoxetine or sertraline, especially at high doses or when first started. It’s less frequent than with antipsychotics, but still happens. If you start an SSRI and suddenly feel an unbearable urge to move, especially in your legs, akathisia should be considered.
Is akathisia the same as Parkinson’s?
No. Parkinson’s from medication (called drug-induced parkinsonism) causes tremors, stiffness, slow movement, and a shuffling walk. Akathisia doesn’t cause stiffness or slowness. It causes an urgent need to move. The two can happen together, but they’re different conditions with different treatments.
How long does akathisia last after stopping the drug?
It depends. Acute akathisia usually improves within days to weeks after stopping the medication. Chronic akathisia lasts over 6 months and may require ongoing treatment. Tardive akathisia can appear months after stopping the drug and may be permanent in some cases. Early intervention improves outcomes.
Can I treat akathisia with over-the-counter supplements?
No. While some people try magnesium, iron, or vitamin B6 for restless legs, these don’t work for akathisia. In fact, taking dopamine-boosting supplements like L-DOPA can make akathisia worse. The only proven treatments are medication adjustments and prescription drugs like propranolol or clonazepam. Always talk to your doctor before trying anything.
Why do doctors miss akathisia so often?
Because it looks like anxiety, agitation, or worsening psychosis. Most doctors aren’t trained to recognize the specific motor signs-like constant leg shifting or pacing during a 10-minute appointment. Also, patients often don’t describe it correctly. They say, "I feel anxious," not, "I have an unbearable urge to move that I can’t control." Better screening tools and education are urgently needed.

Allison Priole
man i wish i knew about this 3 years ago. i was on risperidone and thought i was just "anxious" or "overthinking". turned out i was pacing like a caged tiger for weeks. my doc just kept upping the dose. i felt like i was losing my mind. finally found this thread on reddit and looked up akathisia. holy crap. it was like someone put a name to the hell i was in. i tapered off slowly with my new psychiatrist and within 10 days the urge to move just... vanished. like a switch flipped. i cried. not from sadness. from relief. if you're reading this and feel like your body won't let you sit still? don't ignore it. it's not in your head. it's in your dopamine. and it can be fixed.
Sandy Wells
This article is way too long and overly dramatic. People just need to toughen up. If you can't sit still maybe you're just lazy or have too much caffeine. I've been on antipsychotics for 15 years and I'm fine. Stop making everything a medical emergency.
Chris Dwyer
YES. This is so important. I’m a nurse and I’ve seen so many patients get misdiagnosed. One guy on haloperidol was literally bouncing off the walls and the team kept calling it "psychotic agitation". We finally asked if he felt like his bones were buzzing under his skin and he burst into tears. He said yes. We switched meds. He slept for 12 hours straight that night. Akathisia isn’t a personality flaw. It’s a neurological emergency. If your doc doesn’t know this, find someone who does. You’re not crazy. You’re just being poisoned by the wrong med.
Bryan Woody
Oh great another 10 page essay on how doctors are dumb. Yeah we get it. Akathisia is bad. But you know what’s worse? People who think they know everything after reading one article on Wikipedia. Propranolol? Clonazepam? You’re not a psychiatrist. Don’t self-diagnose. And for god’s sake stop telling people to stop their meds. That’s how you end up in the psych ward. Also pimavanserin? That’s $12,000 a month. Good luck getting that covered. This post reads like a pharmaceutical ad with emotional manipulation. I’m tired of fearmongering disguised as education.
trudale hampton
Just wanted to say thank you for writing this. I’ve been living with this for 7 years. My first episode was after starting sertraline. I thought I had RLS. Took me 2 years to figure out it was akathisia. I’m on olanzapine now and take propranolol daily. It’s not perfect but I can sit through a movie now. If you’re reading this and you’re suffering - you’re not alone. There’s a community out there. You’re not weak. You’re not crazy. You’re just reacting to a drug that doesn’t play fair. Keep fighting.
Shaun Wakashige
lol. i got this. my doc said "you're just jittery". i said "no i feel like my bones are on fire". he laughed. i left. now i'm off meds and doing yoga. 🙏
Paul Cuccurullo
This is one of the most critical, under-discussed tragedies in modern psychiatry. The fact that patients are being misdiagnosed with worsening psychosis - while their very nervous systems scream for relief - is not just a medical failure. It is a moral one. The human cost of this ignorance is incalculable. I weep for the ones who didn’t make it. I weep for the ones still suffering in silence. We must demand better. We must train our clinicians. We must fund research. We must listen. Not because it’s trendy. Because people are dying.
Casey Tenney
Doctors are lazy. They don't want to think. They just prescribe. Akathisia is real. Stop blaming patients. Stop blaming anxiety. It's the drug. End of story.
Timothy Olcott
AMERICA NEEDS TO STOP DOING DRUGS. IF YOU DON'T LIKE THE SIDE EFFECTS THEN DON'T TAKE THEM. I'M A VET. I TOOK ANTIPSYCHOTICS IN THE MILITARY AND I NEVER HAD A PROBLEM. YOU'RE JUST WEAK. 🇺🇸💪
Desiree LaPointe
How quaint. Another amateur psychiatrist with a Google search history and a flair for melodrama. You’ve conflated a common side effect with a narrative of martyrdom. The fact that you’ve elevated akathisia to the level of a Shakespearean tragedy is… charming. But let’s not forget: we live in an age of pharmaceutical overreach, not medical conspiracy. A beta-blocker? Really? That’s your solution? You’re treating a neurological cascade with a band-aid and a prayer. And please, spare us the "I found it on Wikipedia" heroism. We’ve all been there. We’ve all Googled our way out of a crisis. But let’s not pretend ignorance is enlightenment.
Johny Prayogi
Just had my first akathisia episode after starting fluoxetine. I thought I was going crazy. Then I found this. Thank you. I asked my doctor for propranolol and she actually listened. We lowered the dose. I’m sleeping again. I’m not crying every night. This saved me. You’re not alone. I’m here. We’re here. 💙
Nicole James
Of course they don't want you to know this. The pharmaceutical industry profits from misdiagnosis. They know akathisia is underreported. They know doctors are trained to ignore it. They know people will self-medicate with alcohol or opioids because they're too scared to speak up. And now? They're pushing AI tools and apps to "detect" it - but only after you've suffered for years. This isn't medicine. It's surveillance capitalism with a stethoscope. They're monetizing your agony. And they're calling it innovation. Wake up. This isn't about dopamine. It's about control.
Nishan Basnet
I am from India and I work in a psychiatric unit here. We rarely screen for akathisia. Most patients are on first-gen antipsychotics - haloperidol, chlorpromazine. The pacing, the leg shifting - we call it "restlessness" and assume it’s part of the illness. I’ve seen patients who were misdiagnosed for over a year. One man, 52, was on 20mg haloperidol daily. His legs were always in motion. We tried antianxiety meds. Nothing worked. When we finally considered akathisia, we switched to quetiapine and added propranolol. Within 48 hours, he sat through dinner without shifting. He cried. He said, "I didn’t know I could be still." Education is the gap. Not just in the West. Everywhere. Thank you for this. We need more like this.
Jackie Tucker
How predictable. Another long-winded manifesto disguised as clinical insight. You’ve turned a common, well-documented side effect into a cultural crusade. The Barnes Scale? TMS? Pimavanserin? How delightfully performative. You’ve managed to make a pharmacological quirk feel like a revolutionary revelation. How quaint. Did you also write a sonnet about the existential horror of pacing? The truth is, most patients adapt. Most clinicians learn. And most of us? We just want to be treated like adults - not trauma victims in a Netflix documentary.
Thomas Jensen
They’re watching you. The AI tools? The apps? The "movement disorder society"? That’s not medicine. That’s surveillance. They’re tracking your leg movements. They’re recording your pacing. They’re building a database of your discomfort. And soon? They’ll use it to deny you insurance. Or raise your premiums. Or flag you as "high-risk". This isn’t about helping. It’s about control. You think this article is saving lives? It’s just another step toward a world where your body’s natural reactions are pathologized - and monetized. Wake up. They’re not here to help you. They’re here to profit from your pain.