Heartburn is something millions of people deal with every day. For most, it's just an annoying side effect of a spicy meal or a late-night snack. But when that burning sensation becomes a constant part of your life for years, it's no longer just about discomfort. There is a serious biological shift that can happen in your throat that most people ignore until it's too late. The real danger isn't the acid itself, but how your body tries to survive it.
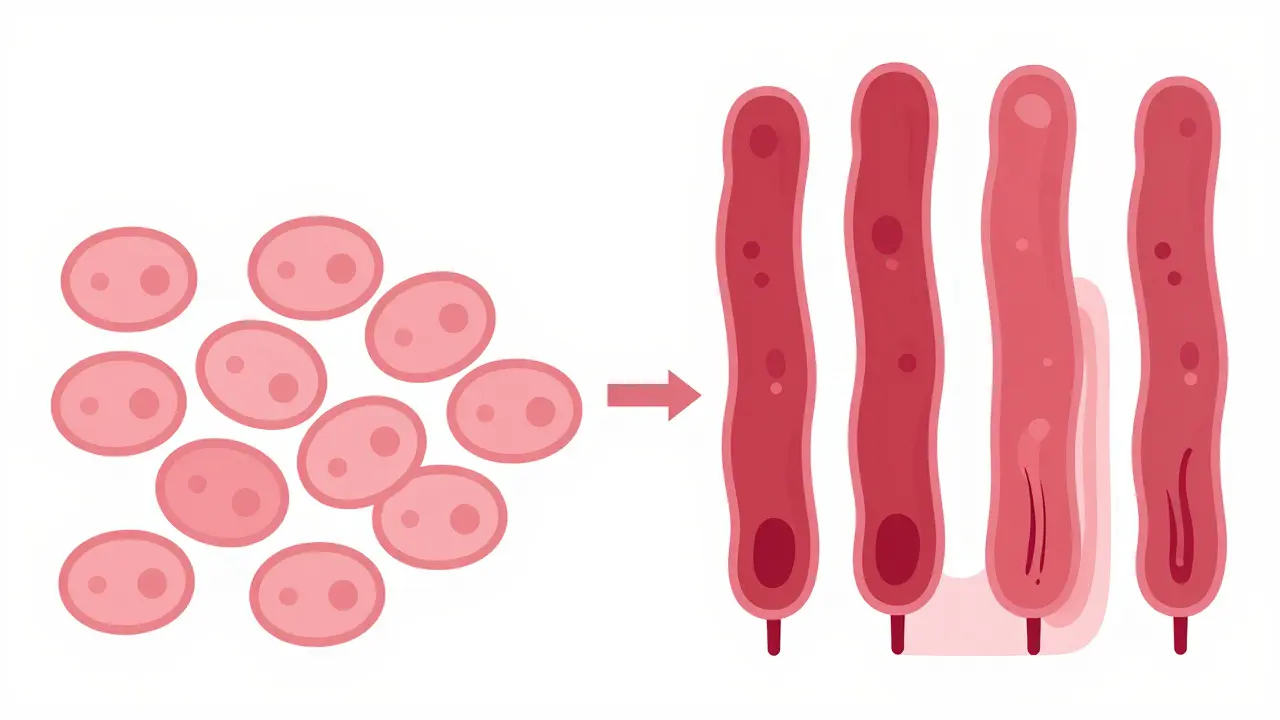
When you have long-term reflux, your body does something clever but risky: it changes the lining of your esophagus to look more like the lining of your stomach. This is because stomach cells can handle acid, while esophageal cells can't. While this adaptation helps with the pain, it creates a precancerous state. If you've had acid reflux for five years or more, you need to understand the bridge between a common stomach issue and a life-threatening malignancy.
The Connection Between GERD and Cancer
To understand the risk, we have to look at Gastroesophageal Reflux Disease is a chronic condition where stomach acid flows back into the esophagus, irritating the lining. Commonly known as GERD, this isn't just "bad heartburn"; it's a persistent assault on your internal tissues.
According to a 2023 study published by the NIH, people with GERD have a 3.20-fold increased risk of developing esophageal cancer. The risk isn't equal for everyone, though. If you experience symptoms weekly, that risk jumps significantly-up to 7 times higher than someone without GERD. This happens because the constant chemical burn from stomach acid forces the cells to mutate to survive.
This mutation leads to Barrett's Esophagus is a condition where the normal squamous epithelium of the esophagus is replaced by columnar epithelium, resembling the intestinal lining. It is currently the only known precursor to adenocarcinoma of the esophagus. Most people with GERD won't develop this-only about 0.5% to 2% of patients do annually. However, once Barrett's is present, the path to cancer becomes a real possibility, with 0.2% to 0.5% progressing to malignancy each year.
Who Is Actually at High Risk?
Not every case of heartburn is a ticking time bomb. However, certain biological and lifestyle factors act as multipliers. If you check three or more of the following boxes, your risk profile changes significantly:
- Gender and Age: Men are 3 to 4 times more likely to develop this cancer than women. Additionally, 90% of all cases occur in people over the age of 55.
- Ethnicity: There is a stark difference in rates; white non-Hispanic individuals have roughly 3 times higher rates of adenocarcinoma than Black Americans.
- Weight: Obesity (a BMI of 30 or higher) increases the risk 2 to 3 times. This is partly because extra abdominal fat puts physical pressure on the stomach, forcing acid upward.
- Lifestyle: A history of smoking increases the risk by 2 to 3 times. When combined with chronic GERD, these risks aren't just added together-they multiply.
| Risk Factor | Estimated Risk Increase | Primary Cancer Type |
|---|---|---|
| Chronic GERD (5+ years) | 3.2x (aHR) | Adenocarcinoma |
| Heavy Alcohol (3+ drinks/day) | 5x | Squamous Cell Carcinoma |
| Smoking History | 2-3x | Both types |
| Achalasia | 16-33x | Squamous Cell Carcinoma |
Red Flags: When to Stop Waiting
The tragedy of esophageal cancer is that 75% of cases are caught at advanced stages. Why? Because people get used to the symptoms. They think, "Oh, it's just my reflux again." But there are specific "red flags" that mean you need to see a doctor immediately.
The most critical warning sign is Dysphagia is difficulty swallowing, often starting with solid foods like meat or bread and eventually progressing to liquids. This symptom is present in 80% of cancer cases at the time of diagnosis. If you feel like food is getting "stuck" in your chest (food impaction), this occurs in about 30-40% of patients and is a major alarm bell.
Other high-priority symptoms include:
- Unexplained Weight Loss: Losing more than 10 pounds in 6 months without trying. This happens in 60-70% of patients.
- Chronic Voice Changes: A hoarse voice or a persistent cough that lasts more than two weeks (found in 20-25% of cases).
- Late-Onset Reflux: If you are over 50 and suddenly develop new or worsening acid reflux, don't just buy over-the-counter meds. Get it checked.

Taking Action and Prevention
The good news is that this isn't an inevitable slide toward cancer. Early intervention can change the outcome. For instance, consistent use of Proton Pump Inhibitors is a class of medications (PPIs) that significantly reduce stomach acid production. Studies show that consistent PPI therapy for over 5 years can reduce cancer risk by up to 70% in patients who already have Barrett's esophagus.
Lifestyle shifts also have measurable impacts. Quitting smoking can slash your risk by 50% within a decade. Even a modest weight loss of 5-10% of your total body weight can reduce GERD symptoms by 40% in obese patients by relieving the pressure on the lower esophageal sphincter.
For those in high-risk groups-specifically white men over 50 with a decade of reflux-the gold standard for prevention is Endoscopy is a procedure where a flexible tube with a camera is used to visualize the esophageal lining. Regular endoscopic surveillance for those with dysplasia can reduce cancer mortality by 60-70%.
The Future of Screening
We are moving away from a "one size fits all" approach to screening. New tools like the "BE MAPPED" risk calculator now help doctors quantify risk with 85% accuracy based on age, BMI, and GERD duration. We're also seeing the rise of non-invasive tools like the Cytosponge-a small sponge on a string that collects cells without needing a full sedative endoscopy. This device has shown nearly 80% sensitivity in detecting Barrett's esophagus.
The goal is shifting toward personalized medicine. Researchers are looking at genetic markers, such as polymorphisms in the CRTC1 gene, which can tell us if a patient is 2 to 3 times more likely to progress from simple reflux to a precancerous state. The earlier we identify these genetic predispositions, the sooner we can start aggressive prevention.
Does everyone with GERD get esophageal cancer?
No. In fact, the vast majority do not. While GERD is common (affecting about 20% of the US population), only 10-15% of chronic GERD patients develop Barrett's esophagus, and only a tiny fraction of those (0.2-0.5% per year) ever progress to cancer.
How long does GERD have to last before it's a risk?
Medical experts generally consider GERD lasting 5 years or more to be a significant risk factor for developing Barrett's esophagus. Those with 10 or more years of symptoms, even if mild, are at a higher risk.
What is the difference between adenocarcinoma and squamous cell carcinoma?
Adenocarcinoma is the type strongly linked to GERD and Barrett's esophagus; it starts in the gland-forming cells of the lining. Squamous cell carcinoma is more closely related to smoking and heavy alcohol use, starting in the flat squamous cells of the esophagus.
Can weight loss actually stop the progression to cancer?
While it may not "reverse" existing Barrett's esophagus, losing 5-10% of body weight reduces the physical pressure on the stomach. This decreases the frequency of acid reflux by about 40%, which reduces the ongoing cellular damage and slows the progression toward malignancy.
When should I insist on an endoscopy?
You should seek an upper endoscopy if you are a white male over 50 with chronic GERD (5+ years) and at least two other risk factors (like obesity or smoking). Also, any appearance of "red flags"-such as difficulty swallowing or unexplained weight loss-should trigger an immediate request for screening regardless of age.
Arthur Luke
The part about the lining changing to survive the acid is honestly wild. It is such a strange biological workaround that ends up being a liability in the long run.
Olushola Adedoyin
Typical big pharma push! They tell you that you need these PPI pills for five years just to stop a cancer that only happens to a tiny fraction of people. It is a total racket to keep us hooked on chemicals that probably mess with our gut biome in ways they won't tell us about! Follow the money, folks, it always leads back to the labs!
Tokunbo Elegbe
It is so important to listen to your body... especially when it comes to these "red flags"... many of us just ignore the signs for too long!!!
Shalika Jain
Imagine being so basic that you actually find this information shocking. Like, we all know that obesity and smoking are bad for you, maybe we don't need a whole table to explain that we're destroying our insides. Truly groundbreaking stuff here, just revolutionary.
Brigid Prosser
Listen up everyone, if you're feeling that food getting stuck, stop playing around and get to a doctor. There's no room for "wait and see" when it comes to your throat. Get the scope, get the answers, and take control of your health before the situation becomes a nightmare. You've got this, just be proactive!
Lynn Smith
I completely agree that the non-invasive tools sound like a great way to make the process less scary for people.
Lesley Wimbush
I've always said that a refined diet is the only real cure, though I'm sure most people here prefer the quick fix of a pill. It's just so typical of the modern mindset to ignore the root cause of the inflammation in favor of a chemical shield. Honestly, if you're not treating your body like a temple, why are you surprised when it starts breaking down? It's almost comical how people ignore the obvious signs of their own poor choices until they're staring at a diagnosis.
Valorie Darling
probs just heartburn lol stop scaring everyone
Charlotte Boychuk
The way the body just adapts and says "fine, I'll be a stomach now" is just a crazy bit of biological improvisation. It's like a makeshift patch that eventually glitches out. I'm just glad there are easier ways to check it now so people don't have to go through the full sedative experience every time.
julya tassi
The Cytosponge sounds so interesting! I wonder if it's widely available in all clinics yet? :)
Wendy Ajurín
It is imperative to note that while PPIs are effective, they should be managed under strict medical supervision to avoid potential long-term side effects. Regular monitoring is the most prudent approach for high-risk individuals.
Truman Media
Life is a journey of learning and caring for the gifts we are given. Let us be kind to ourselves and seek help when the body speaks to us. Peace and health to all! 🌟
William Young
I think the data on weight loss is the most encouraging part of this. It's a practical step that anyone can start today.
Bob Collins
Fair point on the weight loss, but let's be real, some of us have it genetically. Still, getting the endoscopy if you're in that high-risk bracket is a no-brainer. Better to spend an hour in a clinic than a year in a hospital bed. Just a bit of common sense really.